What you need to know when you do not have menstrual periods
So you are not having your cyclical menstrual periods? You might have a condition called Amenorrhea.

Woman with hands on the front of her lower abdomen. Click on image to enlarge.
Introduction
Amenorrhea is the medical term used to describe the absence of menstrual periods that is either permanent or temporary. It may be primary or secondary.
The aim of this resource is to provide you with accurate information to help you know why you do not have your menstrual periods and what you can do about it. Read on.
Types of amenorrhea
There are two broad types of this condition.
- Primary amenorrhea - this is the absence of menstrual bleeding in a girl (by age 16 years) with normal development of secondary sexual characteristics.
- Secondary amenorrhea - this is the absence of menstrual bleeding in a woman who had been menstruating but later stops menstruating for at least three consecutive months in the absence of pregnancy, lactation (production of breast milk), use of hormonal birth control pills, or menopause.
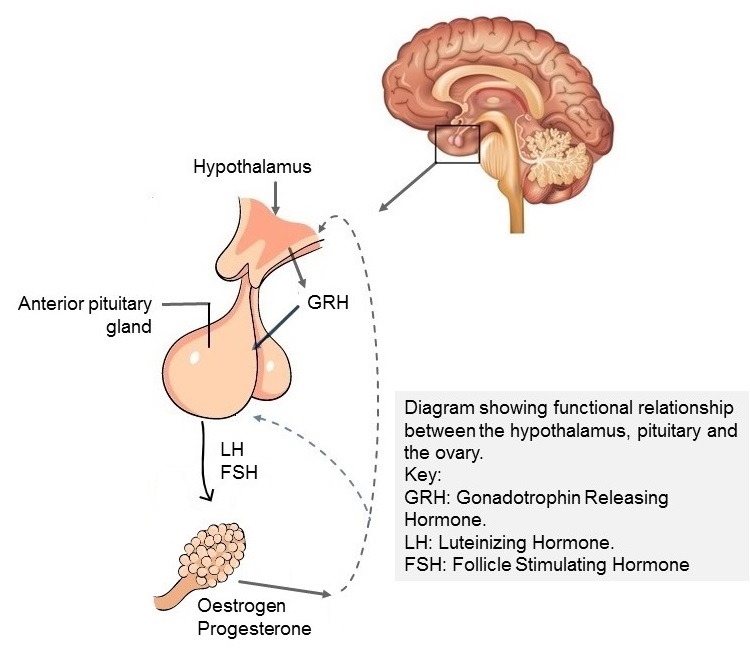 For a woman to have regular menstrual cycles, certain regions of her brain (i.e., the hypothalamus and pituitary gland, must be functioning normally. In addition, her reproductive organs like the ovaries and uterus should all be functioning normally.
For a woman to have regular menstrual cycles, certain regions of her brain (i.e., the hypothalamus and pituitary gland, must be functioning normally. In addition, her reproductive organs like the ovaries and uterus should all be functioning normally.
The hypothalamus is a part of the brain that stimulates the pituitary gland to release specific chemicals called hormones (e.g., follicle-stimulating hormone (FSH) and luteinizing hormone (LH)). These hormones cause the ovaries to produce additional hormones (i.e., estrogen (oestrogen) and progesterone).
Estrogen and progesterone are responsible for the cyclical changes in the uterine lining that causes menstrual periods to happen. This assumes that the woman’s genital tract is free of abnormalities to allow the free passage of the menstrual blood.
Click here to view a summary of amenorrhea facts
Causes of Amenorrhea
The causes of amenorrhea can be grouped under the following:
- Undiagnosed pregnancy.
- Abnormalities in the hypothalamic-pituitary-ovarian axis.
- Reproductive tract anatomical abnormalities.
- Other functional causes.
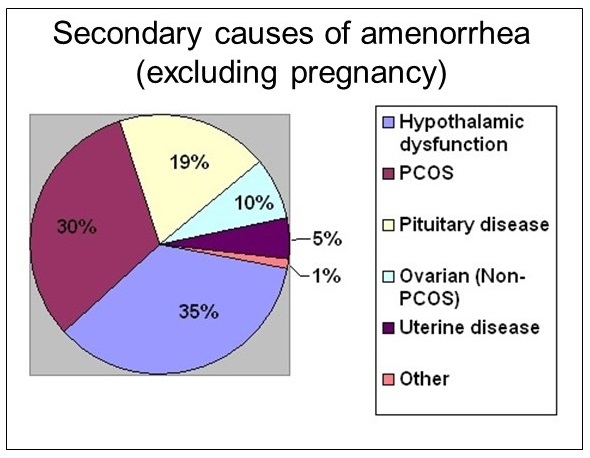
Diagram showing secondary causes of amenorrhea. Click on image to enlarge.
Common hypothalamic causes of amenorrhea include:
- A brain tumor near the pituitary gland (e.g. Craniopharygioma)
- Deficiency of pituitary hormones that promote growth and function of the ovaries and uterus (e.g., Kallman syndrome)
- Dietary/nutritional deficiency
- Low body weight or growth delay
Common pituitary causes of amenorrhea include:
- High blood levels of a hormone (prolactin) that stimulates secretion of milk from the breasts during breastfeeding. This may possibly be caused by a tumor of the pituitary gland secreting the hormone prolactin).
- Disorders related to other pituitary tumors.
- Death of cells of the pituitary gland after a woman delivers a baby.
- Autoimmune destruction of cells of the pituitary gland by the body’s own defense system.
- A tumor within the pituitary gland (Pituitary adenoma)
- Irradiation of the pituitary
- Other generalized disease which may affect the pituitary (e.g., sarcoidosis)
Common reproductive organs related causes of amenorrhea include:
- Lack of the release of an egg (anovulation).
- Genetic disorder causing underdeveloped ovaries, failure to menstruate, and short stature (e.g., Turner’s syndrome).
- High blood levels of male hormones in a female (Hyperandrogenemia).
- Hormonal disorder affecting women of reproductive age due to Polycystic ovary syndrome (PCOS).
- Premature ovarian failure.
- Primary defective development of the ovary.
- Autoimmune destruction of cells of the ovaries, caused by the body’s own defense system.
- Drugs or Radiation
- Anatomical abnormalities of the genital tract
- Imperforate hymen (i.e., a hymen in which there is no opening, the membrane completely closes off the vagina)
- Transverse vaginal septum (a dividing wall or membrane in the vagina)
- Absent vagina, cervix, and/or the uterus
- Intrauterine adhesions
Common functional causes include:
- Eating disorders like Anorexia/Bulimia
- Chronic diseases (for example, Tuberculosis (Tb))
- Excessive weight gain or weight loss
- Malnutrition
- Psychiatric disorders like depression and anxiety
- Substance abuse
- Medication use (e.g., drugs prescribed to stabilize or improve mood, mental status, or behavior
- Use of hormonal birth control pills or injections.
- Systemic disorders (e.g. hypothyroidism)
- Excessive stress (financial, work related interpersonal, etc.).
- Excessive exercise.
Symptoms of Amenorrhea
Amenorrhea is a symptom of an underlying disorder rather than a disease in and of itself. Therefore, symptoms present in amenorrhea may depend on the associated condition.
Primary or secondary amenorrhea is considered to be present when:
- a girl has not developed menstrual periods by age 16; or
- a woman who has previously had her menstrual cycles and is not pregnant, stops having menstrual periods for at least three consecutive cycles or for a time period of six months or more..
Other symptoms and signs may be present as follows:
- Breasts milk production in a woman who is not pregnant or breastfeeding, coupled with headache and reduce peripheral vision can be a sign of an intracranial tumor.
- Male pattern increased hair growth (hirsutism) may be caused by excess male hormone (androgen) that encourages development of male sex characteristics.
- Vaginal dryness, hot flushes, night sweats and disordered sleep may be a sign of ovarian insufficiency or premature ovarian failure.
- Noticeable weight gain or weight loss may be present.
- Excessive anxiety or depression may be present in women with associated psychiatric abnormalities.
When to Seek Medical Care
1. Consult a health care professional if a girl is 14 years old and her secondary sexual characteristics (for example, breast development and pubic hair) have not started to develop, or a girl is 16 years old and has not had her first menstrual period.
2. For women who have already begun menstruating, they should see a health care professional if they have missed three consecutive menstrual periods.
Diagnosis of Amenorrhea
After taking a good history and performing physical examination, a doctor may perform the following tests to determine the cause of the amenorrhea:
- Blood tests. These may be performed to determine the levels of hormones secreted by the pituitary gland (FSH, LH, TSH, and prolactin) and the ovaries (estrogen).
- CT scan or ultrasonography of the pelvis. These may be performed to assess the abnormalities of the genital tract or to look for polycystic ovaries.
- CT scan or MRI of the head. Either of these may be performed to exclude pituitary and hypothalamic causes of amenorrhea.
If the above tests are inconclusive, the following additional tests may be performed:
- Thyroid function tests
- Determination of prolactin levels
- Hysterosalpingogram (X-ray test) or saline infusion sonography (SIS), both of which examine the uterus
- Laparoscopy or Hysteroscopy (visual inspection of the pelvic organs and uterine cavity respectively)
Treatment of Amenorrhea
Non-medication
- Diet. Where nutritional deficiencies induced by dieting is established as a cause amenorrhea, then recommending a properly balanced diet is appropriate.
- Weight loss. In some women, excessive body weight can be the cause of amenorrhea. Such women should restrict the amount of fat in their diet, and they should exercise moderately and regularly to maintain an ideal body weight.
- Moderate exercise. More than 8 hours of vigorous exercise a week may cause amenorrhea. Initiating a moderate exercise program may help to restore normal menstruation.
- Psychotherapy. In women with eating disorders, or excessive weight loss, normal menstrual cycles can often be restored by undergoing appropriate psychological treatment to restore and maintain a healthy body weight.
- De-stress. If amenorrhea is caused by emotional stress of whatever nature, finding ways to deal with stress and conflicts may help.
- Lifestyle changes. Maintaining a healthy lifestyle by avoiding cigarette smoking, alcohol consumption and recreational drug use is also helpful.
Medication
Medical treatment of amenorrhea will depend on its cause.
Once the cause is determined, treatment is tailored to correcting the underlying disease, and the expectation is that such medication use will restore menstruation.
In case of anatomical abnormalities of the genital tract, surgery may be indicated.
Examples of medications used in the treatment of some causes of amenorrhea include:
- Dopamine agonists such as bromocriptine (Parlodel) or pergolide (Permax), are effective in treating hyperprolactinemia. In most women, treatment with dopamine agonists medications restores normal ovarian endocrine function and ovulation.
- Hormone replacement therapy consisting of an estrogen and a progestin can be used for women in whom estrogen deficiency remains because ovarian function cannot be restored.
- Metformin (Glucophage) has been successfully used in women with polycystic ovary syndrome (PCOS) to induce ovulation.
- Oral contraceptives may be prescribed in some cases to restore menstrual cycle and to provide estrogen replacement to women with amenorrhea who do not wish to become pregnant.
Surgical options for Amenorrhea
- If a pituitary or hypothalamic tumor is established, surgery and in some cases, radiation therapy may be indicated.
- Women with intrauterine adhesions require dissolution of the scar tissue.
- Surgical procedures required for other genital tract abnormalities depend on the specific clinical situation.
Amenorrhea Follow-up
Women with amenorrhea caused by ovarian insufficiency require follow-up. This is implemented to check the effectiveness of ovarian hormone replacement and to detect the development of any adverse conditions.
Prevention of Amenorrhea
Some secondary causes of amenorrhea may be prevented where appropriate. For example, maintaining a normal weight, can prevent primary amenorrhea caused by excessive weight loss or weight gain
Amenorrhea Prognosis
Amenorrhea is typically not a life-threatening condition. The prognosis for amenorrhea depends upon the underlying cause and the type of treatment that is available. For most women, medications, lifestyle changes, or surgery can correct amenorrhea.
Reduced bone density and increase in bone fracture rates has been associated with prolonged amenorrhea.
Related professional resource: Amenorrhea: Evaluation and Treatment
Published: March 1, 2020
Last Update: November 12, 2023
© 2020 - 2024. Datelinehealth Africa Inc. All rights reserved.
Permission is freely given to copy, use and share content for non-commercial purposes, without alteration or modification and subject to source attribution.
 For a woman to have regular menstrual cycles, certain regions of her brain (i.e., the hypothalamus and pituitary gland, must be functioning normally. In addition, her reproductive organs like the ovaries and uterus should all be functioning normally.
For a woman to have regular menstrual cycles, certain regions of her brain (i.e., the hypothalamus and pituitary gland, must be functioning normally. In addition, her reproductive organs like the ovaries and uterus should all be functioning normally.