Why African Girls Need the HPV Vaccine
By Chika Jones RN RM RPHN BNSC Freelance Health Writer. Medically reviewed by the DLHA Team.

A black nurse withdrawing vaccine from a vial into a syringe. Image source: Freepik
Human Papillomavirus (HPV) is the main cause of cervical cancer. HPV has over 100 subtypes. Low-risk HPV (HPV 6 and 11) causes genital warts, while high-risk HPV (HPV 16 and 18) causes cervical cancer [1]. Cervical cancer affects women irrespective of background, race, and economic status. Cervical cancer is a major health threat affecting sub-Saharan Africa women. HPV vaccination is crucial for African girls to prevent cervical cancer and promote health.
This article explores the importance of HPV vaccination for African girls, factors influencing vaccine uptake, and strategies to promote vaccination in Africa.
A picture explaining Human Papillomavirus. Click on image to enlarge. Image source: Freepik
HPV is transmitted through sexual contact. Most HPV infections resolve on their own within two years without noticeable symptoms. However, persistent infections with high-risk HPV types such as HPV 16 and 18 can lead to abnormal cell growth in the cervix. If left untreated, these abnormal cells can develop into cancer and potentially spread to other parts of the body [2].
HPV is associated with a range of health issues beyond cervical cancer including:
Types of HPV Vaccine
WHO licensed six HPV vaccines to be used globally. They are shown in table 1 below.
Table 1. Detailing available HPV vaccines. Click on image to enlarge. Source.
Cervarix, Gardasil, and Gardasil-9 are currently available in sub-Saharan Africa. Cervarix protects against two HPV types that cause cancer. Gardasil protects against four HPV types that cause cancer and genital warts. Gardasil 9 protects against nine HPV types, covering both cancer-causing and wart-causing strains.
There are 12 high-risk types of HPV 31, 33, 45, 52, and 58. These types could also cause cervical cancer but HPV 16 and 18 are more likely to cause HPV-related cancers [1].
The HPV vaccine triggers production of antibodies that recognize and destroy HPV. This prevents HPV from entering cells [3].
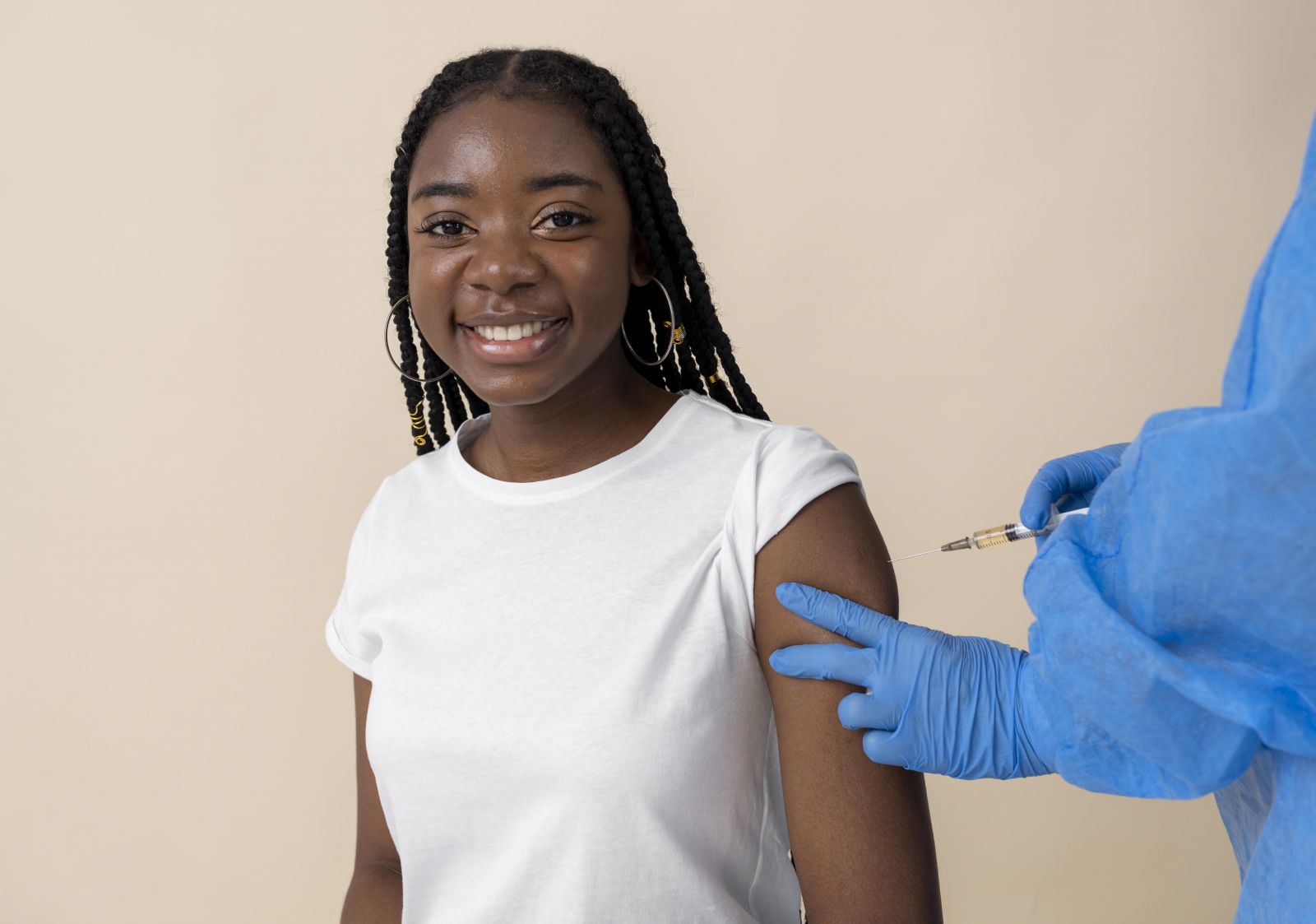
An image of a girl receiving vaccination Image source: Freepik
African women who engage in sexual activity may contract HPV unknowingly, and the HPV vaccine may not treat it. Hence, WHO recommends the HPV vaccine for adolescent girls aged 9-14 before they engage in sexual activity.
The World Health Organization (WHO) has updated its HPV vaccination recommendations as shown in Table 2 below:
Table 2: WHO recommended HPV vaccination schedule. Click on image to enlarge. Source: WHO. 2022
HPV vaccines are available in Africa but it is not being fully implemented. Findings reveal that HPV vaccination coverage in sub-Saharan Africa is 20%. Let us discuss the challenges of HPV vaccination and possible solutions.
Solution: Awareness campaigns must be held in schools to educate African girls on HPV vaccination. Research shows that individuals with knowledge about HPV vaccination increased their compliance.
Community outreaches must be done to educate African women and mothers about HPV vaccination for themselves, their sisters, and their daughters. Mass media exposure on the radio, television, and the internet must be done to sensitize the public about HPV vaccination.
African mothers may not be worried about cervical cancer and its related diseases and they could believe that their daughter would wait and there's no need for her to take the vaccination.
Solution: Healthcare professionals should counsel mothers to let their daughters receive the HPV vaccine as it protects them from future harm.
These conditions may not readily be available in some African countries, leading to poor uptake of HPV vaccination.
Solution: The structural challenges must be identified and resolved to improve African girls' safe uptake of HPV vaccination.
They may have beliefs that the vaccination would make their daughters more promiscuous or they may be worried about potential side effects.
Solution: Community outreaches should be engaged respecting community culture and beliefs to dispel myths or misconceptions about HPV vaccination.
Solution: School-based HPV vaccination could be implemented to ensure every African girl receives it with parental consent. Healthcare facilities should be readily available and accessible in African rural areas.
Cervical cancer is an eminently preventable disease through HPV vaccination. Most African women may have cervical cancer and not even know until it’s too late for a good treatment outcome. For this reason and more, it is very essential for every African girl and woman to be vaccinated for HPV. While factors such as lack of awareness, misinformation and socioeconomic status conditions could affect HPV vaccination uptake among African girls, addressing cultural and infrastructural challenges, and implementing effective communication strategies, can help lower parental resistance for African girls to be vaccinated against HPV.
Related:
Cervical Cancer: What African Women Need to Know
Cervical Cancer Screening Information for African women
Published: August 23, 2025
© 2025. Datelinehealth Africa Inc. All rights reserved.
Permission is given to copy, use and share content freely for non-commercial purposes without alteration or modification and subject to source attribution
DATELINEHEALTH AFRICA INC., is a digital publisher for informational and educational purposes and does not offer personal medical care and advice. If you have a medical problem needing routine or emergency attention, call your doctor or local emergency services immediately, or visit the nearest emergency room or the nearest hospital. You should consult your professional healthcare provider before starting any nutrition, diet, exercise, fitness, medical or wellness program mentioned or referenced in the DatelinehealthAfrica website. Click here for more disclaimer notice.