By: Foluke Akinwalere. Freelance Health Writer. With medical review and editorial support by the DLHA Team.

Black lady with facial skin condition. Image by Freepik
In Africa, the burden of skin diseases is significant, with prevalence patterns varying across different regions and countries. While some skin diseases are endemic to specific geographical areas, others exhibit widespread distribution throughout the continent.
Despite the diversity in prevalence, skin diseases share common themes of impacting individuals’ physical health, psychological well-being, and socio-economic status.
This article aims to provide insight into the prevalence, clinical features, and management of five skin diseases that are common among Africans, drawing attention to the importance of tailored interventions to address regional variations and promote skin health in diverse African populations.
Acne vulgaris, also known simply as acne, is a chronic inflammatory skin condition that commonly manifests with pimples, papules, pustules, blackheads, whiteheads, nodules, and cysts. It primarily affects the face, chest, upper arms, and back. These lesions can be painful, and inflamed, and may leave scars if not treated properly.
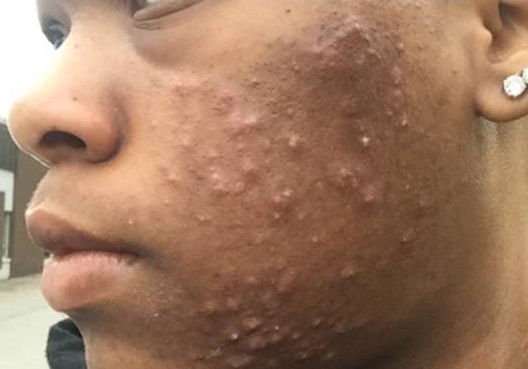
Man with facial acne
Acne vulgaris affects people of all ethnicities, including African populations. While there may be variations in the prevalence and severity of acne among different ethnic groups, it is a common dermatological concern worldwide.
Acne vulgaris has been reported to account for 4.6% of skin disease cases in Ghana, 6.7% in Nigeria, and as high as 17.5% in South Africa, according to hospital-based studies in Africa. [1]
Several factors contribute to the development of acne vulgaris, including:
Preventive measures for acne vulgaris include maintaining good skincare habits such as:
Eczema, also known as atopic dermatitis, is a long-lasting skin condition that is characterised by dry, itchy, and inflamed patches of skin. It is often accompanied by redness, swelling, and sometimes the formation of small fluid-filled blisters. The period when the disease gets worse is called “flares”. [3] It can persist for years, even throughout one’s lifetime,
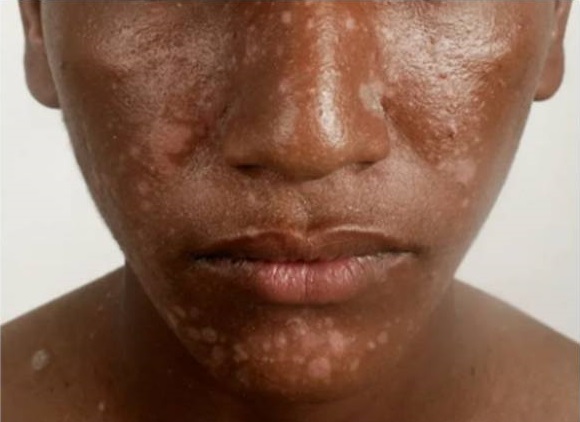
Black man with facial eczema (atopic dermatitis)
The most common symptom of eczema is itching, and scratching can lead to further:
While prevalence rates may vary among different ethnic groups, eczema can have a significant impact on the quality of life, causing discomfort, and affecting sleep and daily activities. It is a common condition that usually begins in childhood; however, anyone can get the disease.
Eczema impacts as many as 20% of children and 3% of adults, with recent worldwide data, indicating a rise in its prevalence. In Africa, the occurrence of eczema varies from 4.7% to 23%. [4]
It typically starts between 2 and 6 months of age, but it can start at any age. It was previously believed that it usually goes away by adulthood, but there is evidence to suggest that it is a long-lasting condition that can continue in adulthood.
Treatment options for eczema include:
Keloids are benign, raised scars that extend beyond the boundaries of the original wound or injury. They are characterised by excessive collagen production during the wound healing process, resulting in raised, firm, and sometimes shiny or lumpy scar tissue. It may develop as early as 1 to 3 months or as late as one year after injury. [5]
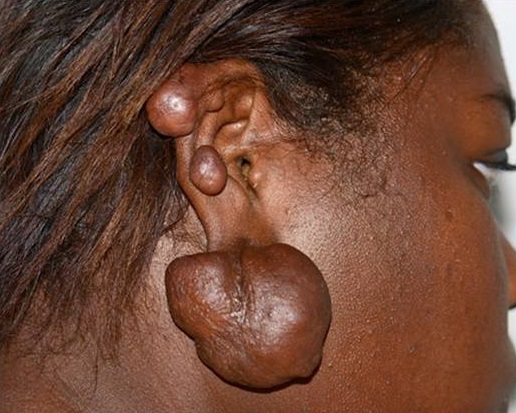
Black woman with right earlobe keloids
Keloids are more common in individuals of darker-skinned Africans. This suggests that there may be a genetic proneness to keloid formation in African populations.
The average keloid incidence is estimated to be 5–10% in African countries, compared to 0.1% in Asian countries, and less than 0.1% in other countries. [6]
Keloids often develop following trauma or injury to the skin, such as surgical incisions, burns, acne scars, or piercings. Genetic factors such as family history, and individual tendencies, such as skin type and hormone levels also play a role in keloid formation.
This depends on several factors such as the size of the keloid, their location, the age of the patient, and how old the keloid is.
Keloid treatments include:
Combination therapies may be used to achieve better outcomes. However, keloids have a high recurrence rate, and no single treatment is universally effective.
Tinea (dermatophytosis), commonly known as ringworm, refers to a group of fungal infections affecting the skin, scalp, and nails. It is characterised by ring-shaped, red, scaly patches with clearing centers.
Around 40 various species of fungi are capable of causing ringworm; the scientific names for the fungi that cause ringworm are Trichophyton, Microsporum, and Epidermophyton. [7]
There is an increased risk of contracting tinea infections if a person:
The different types of tinea are usually named for the location of the infection on the body.
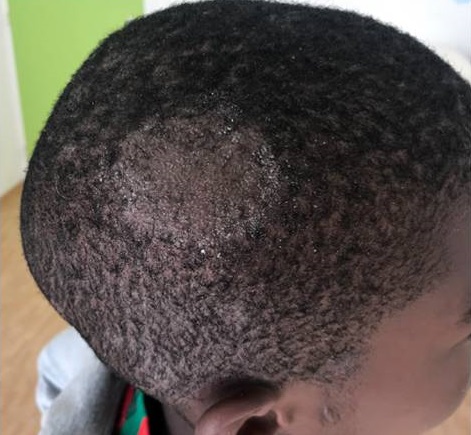
African boy with tinea capitis infection of the right scalp
It is a fungal infection of the scalp and hair follicles. Tinea capitis is prevalent in African communities, particularly among children.
The 2019 United Nations Population data was used to determine the number of children at risk of tinea capitis in each African country. With a population of 600 million children, the estimated total number of tinea capitis cases in Africa was 138.1 million. Sub-Saharan Africa alone accounted for over 96% (132.6 million) of these cases. [8]
It is highly contagious. The symptoms of tinea capitis include:
Tinea capitis risk factors include poor hygiene and close contact with infected individuals. Treatment typically involves antifungal medications, both topical and oral.
Tinea capitis preventive measures include maintaining good hygiene, avoiding sharing personal items like combs or hats, and prompt treatment of infected persons.
Tinea corporis, or ringworm of the body, affects the skin on the body excluding the scalp, groin, and feet. It affects all ages but is more common in children.
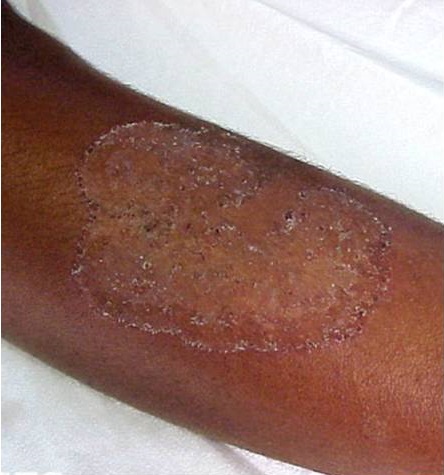
Tinea corporis infection of the skin in ablack individual
It spreads through direct contact with infected people or animals or by touching contaminated objects. Symptoms include red, scaly, itchy patches on the skin.
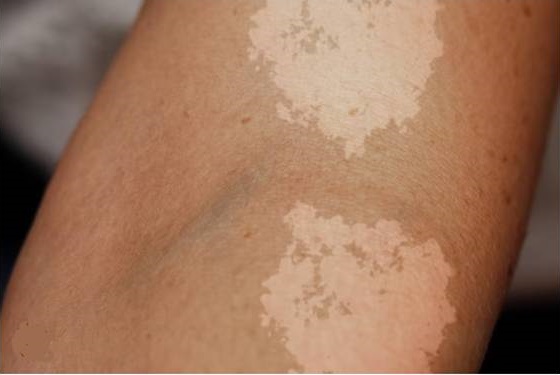
Tinea versicolor in a black individual
This fungal infection, also known as pityriasis versicolor, primarily affects the skin. It is caused by the overgrowth of a type of yeast called Malassezia furfur. Tinea versicolor typically manifests as discolored patches on the skin, often lighter or darker than the surrounding skin.
These patches can be white, pink, tan, or brown and may be more noticeable after sun exposure. It commonly affects areas of the body with a high density of fat or oil, such as the neck, chest, back, and upper arms.
It often affects adolescents and young adults. Its symptoms include patches of skin that may be lighter or darker than the surrounding skin.
Though tinea versicolor and vitiligo can cause changes in skin pigmentation, but they have different causes, characteristics, and treatment approaches. Tinea versicolor is caused by a yeast infection and results in patches of lighter or darker skin that may be itchy or flaky, while vitiligo is an autoimmune condition that causes white patches of skin due to the destruction of melanocytes.
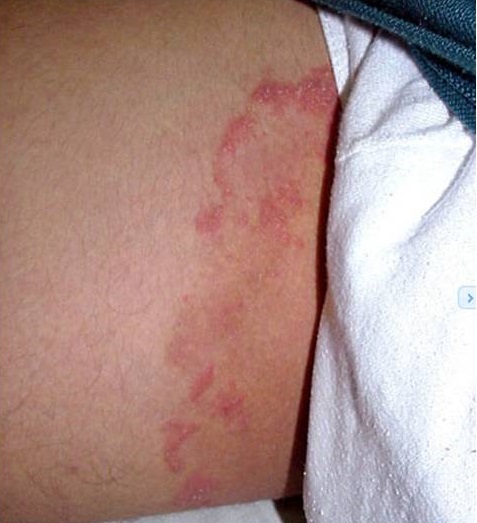
Tinea cruris infection of the groin in a black indivdual.
Tinea cruris, or jock itch, is a fungal infection affecting the groin area. This condition is more common in males than females and happens more often during warm weather conditions. It may be hard to cure.
Tinea cruris is characterised by redness, itching, and a raised rash in the groin folds, inner thighs, and genital area. Tinea cruris risk factors include warm, humid environments, sweating, and wearing tight clothing.
Treatment and preventive measures for tinea infections
Vitiligo is a chronic autoimmune disorder that causes hypopigmented patches on the skin. This happens when melanocytes (skin cells that produce pigments) are attacked and destroyed, causing the skin to turn a milky-white color. [9] These patches can occur anywhere on the body and vary in size and shape.

Black woman with vitiligo
Vitiligo affects individuals of all ethnicities, including Africans. In some African communities, it may be more prevalent due to genetic and environmental factors.
Studies show that the prevalence of vitiligo was as high as 2.5% in Africa, compared with 1.6% in Asia and 1.5% in America. These results were in accordance with previous studies that vitiligo frequently occurred in darker-skinned individuals. [10]
Scientists believe that the cause of Vitiligo is an autoimmune disease in which the body’s immune system attacks and destroys the melanocytes. Family history and genes also play a role in causing vitiligo.
Risk factors of vitiligo involve a combination of genetic, autoimmune, and environmental factors - such as sunburn, emotional distress, or exposure to a chemical - that can trigger vitiligo or make it worse.
Vitiligo is not life-threatening or contagious, but it can have a social and psychological impact on affected individuals. It may also affect quality of life and interpersonal relationships.
This includes medical intervention like topical corticosteroids, phototherapy, and surgery procedures such as skin grafting or melanocyte transplantation. Cosmetic interventions like make-up and self-tanning products may also help.
People with vitiligo require support such as education, counseling, support groups, and advocacy organisations. Coping strategies for them may include developing resilience, self-acceptance, and focusing on overall well-being rather than solely on skin appearance.
Public and private stakeholders in health need to:
Implement community-based educational initiatives such as workshops and seminars, to increase awareness about common skin diseases, such as acne, eczema, keloids, ringworm, vitiligo and other skin diseases within African communities.
Advocate for improved access to dermatological care and services in African communities, particularly in underserved areas. This may involve partnering healthcare providers, community organisations, and policymakers to address barriers to healthcare access, such as affordability, transportation, and cultural beliefs. By expanding access to dermatological services, individuals can receive timely diagnosis, treatment, and support for their skin health needs.
Establish support networks and resources for individuals affected by skin diseases in African communities, offering a platform for sharing experiences, accessing information, and seeking emotional support. This can include online forums, peers support groups, and community-based organisations focused on promoting skin wellness.
In conclusion, the common skin diseases discussed, showcase the diverse range of dermatological conditions that can affect individuals of all ages and ethnicities in Africa. Each condition presents unique features, challenges and considerations, from genetic predispositions to environmental triggers. Awareness and good knowledge of these conditions is crucial for effective diagnosis, treatment, and management, as well as for promoting skin health and overall well-being withAfrican communities.
1. Husain Y. Acne Vulgaris in Nigerian Adolescents – prevalence, severity, beliefs, perceptions, and practices. International Journal of Dermatology. April 9, 2009. Available from: https://onlinelibrary.wiley.com/doi/full/10.1111/j.1365-4632.2009.03922.x
2. Sutaria AH, Masood S, Saleh HM, et al. Acne Vulgaris. [Updated 2023 Aug 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459173/
3. National Institute of Arthritis and Musculoskeletal and Skin Disease. Atopic Dermatitis. Last reviewed: November 2022. Accessed: February 6, 2024. Available from: https://www.niams.nih.gov/health-topics/atopic-dermatitis.
4. Sendrasoa FA, Ranaivo IM, Razanakoto NH et al. Epidemiology and associated factors of atopic dermatitis in Malagasy children. Allergy Asthma Clin Immunol 16, 4 (2020). https://doi.org/10.1186/s13223-019-0398-2
5. McGinty S, Siddiqui WJ. Keloid. [Updated 2023 Jul 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507899/
6. Chenyu H, Zhaozhao W, Yanan D, Rei O. The Epidemiology of Keloids Textbook on Scar Management 2020 ISBN : 978-3-030-44765-6
7. Centers For Disease Control and Prevention. About Ringworm. [Internet. Page Last Reviewed February 29, 2021]. Accessed: February 7, 2024.Available from: https://www.cdc.gov/fungal/diseases/ringworm/definition.html
8. Bongomin F, Olum R, Nsenga L, Namusobya M, Russell L, de Sousa E, Osaigbovo II, Kwizera R, Baluku JB. Estimation of the burden of tinea capitis among children in Africa. Mycoses. 2021 Apr;64(4):349-363. doi: 10.1111/myc.13221.
9. National Institute of Arthritis and Musculoskeletal and Skin Diseases. Vitiligo. [Internet. Last Reviewed: October 2022]. Accessed: February 7, 2024 . Available from: https://www.niams.nih.gov/health-topics/vitiligo
10. Zhang Y, Cai Y, Shi M, Jiang S, Cui S, Wu Y, Gao XH, Chen HD. The Prevalence of Vitiligo: A Meta-Analysis. PLoS One. 2016 Sep 27;11(9):e0163806. doi: 10.1371/journal.pone.0163806.
Acne: Causes, Types, Symptoms, Prevention and Treatment
Common hair and skin problems and how to treat them
Published: February 14, 2024
© 2024. Datelinehealth Africa Inc. All rights reserved.
Permission is given to copy, use and share content freely for non-commercial purposes without alteration or modification and subject to attribution as to source.
DATELINEHEALTH AFRICA INC., is a digital publisher for informational and educational purposes and does not offer personal medical care and advice. If you have a medical problem needing routine or emergency attention, call your doctor or local emergency services immediately, or visit the nearest emergency room or the nearest hospital. You should consult your professional healthcare provider before starting any nutrition, diet, exercise, fitness, medical or wellness program mentioned or referenced in the DatelinehealthAfrica website. Click here for more disclaimer notice.